 
Retinal re-detachment: Despite what seemed like initial successful surgery, the retina can become detached again. 
LATE RETINAL DETACHMENT SURGERY COMPLICATIONS 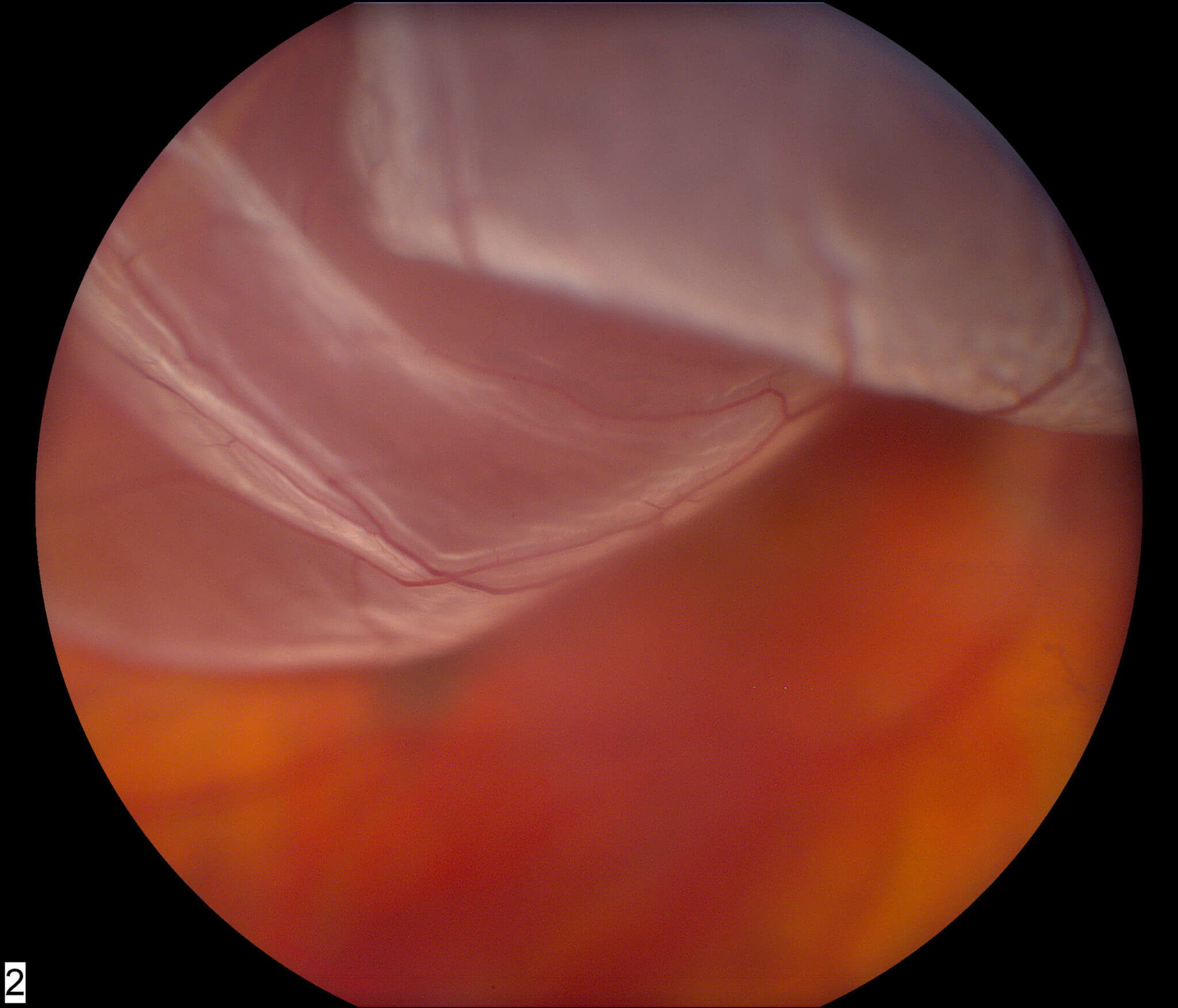
If you have a condition that lowers your immune system and predisposes towards infection, highlight it to your ophthalmologist so that even more precautions can be taken to prevent infection. Luckily, this condition is very rare (less in 0.1%) due to the meticulous cleaning and infection control techniques. Note the yellow fluid level or hypopyon in this eye. This is infection affecting the entire eye, and if not treated expediently with antibiotic injections into the vitreous cavity, will result in permanent blindness. Postoperative infective endophthalmitis is one of the worst possible retinal detachment surgery complications that can occur. However, it can take several months before the eye settles down. The earlier treatment is started, the better the chances of retaining good vision. You will most likely be admitted to hospital for intensive eyedrops and oral medications. Your eye needs immediate injection of antibiotics into the eyeball. This condition is an ophthalmic EMERGENCY, so please do not wait and see "if it gets better over the next few days". There may be yellow discharge from the eye and you may even see a yellow fluid level in the eyeball ( hypopyon). How would you know if you have endophthalmitis? Well, your eye will be extremely painful and you will have very poor sight. It is extremely serious, and you can lose your vision permanently. Infection of the eyeball (endophthalmitis): Endophthalmitis is one of the most dreaded complications of any ocular surgery surgery. This is very painful and bad for your optic nerve. Flying causes the gas in your eye to expand and increase the eye pressure tremendously. If you had gas inserted into the vitreous cavity of your eyeball, you must not to go on any flights for the next few weeks after surgery. Measurement of the intraocular pressure is important during the postoperative period after surgery. This usually does not cause any lasting damage unless the eye pressure is elevated to a very high level or if you already suffer from glaucoma. Depending on how high the eye pressure is, your ophthalmologist may give you eye drops or tablets to bring the pressure down. The raised pressure is usually temporary. If the pressure increase is high, you may experience blurring and aching around the eye, as well as nausea and sickness. Increased pressure in the eye (raised intraocular pressure): This can be uncomfortable, and happens in around 10% of the time. 
In general, retinal detachment surgery complications can be classified into early (within 2 weeks of surgery) and late (after 2 weeks postoperatively) complications.ĮARLY RETINAL DETACHMENT SURGERY COMPLICATIONS Doing so reduces the risk of complications and increases the chance of success of your operation. It is important that you listen and adhere to the advice given to you by your ophthalmologist regarding your eye drops and general care after surgery. Some complications are more difficult to manage than others, and may require repeat surgery and/or frequent outpatient visits. Most of the time, you will have a good outcome if any retinal detachment surgery complications are dealt with promptly and managed properly. The later you postpone surgery, the greater the chances of surgical failure due to scarring from proliferative vitreoretinopathy. The success rates are higher the earlier surgical repair is performed. The only way to fix a retinal detachment (example on the left) is to undergo retinal detachment surgery. If your detached retina is not repaired, you will eventually lose all your visual function in that eye. This is similar to when the wallpaper peels away from your living room wall. When you develop a retinal detachment, your retina (or more specifically, your neurosensory retina) becomes peeled off from the wall of the eye. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
